Hong
Kong Med J 2017 Dec;23(6):653.e3–4
DOI: 10.12809/hkmj165051
© Hong Kong Academy of Medicine. CC BY-NC-ND 4.0
PICTORIAL MEDICINE
Cutaneous manifestation mimicking Stevens-Johnson
syndrome in a critically ill patient: looks similar but totally different
Jo A Lim, MD, MRCP, D Derm1; SE Chong,
MD, MMed2,3; Huda Zainal Abidin, MD, MMed3; Mohd H
Hassan, MBBS, MMed3
1 Department of Internal Medicine,
Hospital Sultan Abdul Halim, 08000 Sungai Petani, Kedah, Malaysia
2 Regenerative Medicine Cluster, Advanced
Medical and Dental Institute, Universiti Sains Malaysia, Bertam, 13200
Kepala Batas, Penang, Malaysia
3 Department of Anesthesiology and
Intensive Care, School of Medical Sciences, Universiti Sains Malaysia,
16150 Kota Bharu, Kelantan, Malaysia
Corresponding author: Dr SE Chong (sechong@usm.my)
Case
A 60-year-old gentleman was intubated due to severe
leptospirosis and multi-organ failure: acute kidney injury and liver
failure with disseminated intravascular coagulation (DIC). He was
ventilated in the intensive care unit for 7 days. He was treated with
ceftriaxone, pantoprazole, fentanyl, midazolam, and required frequent
fluid challenge and inotropic support.
On the day of extubation, the patient was noted to
have ulcers over the angles of the mouth with crusted blood and
seropurulent discharge (Fig 1). He also had diffuse erythema and
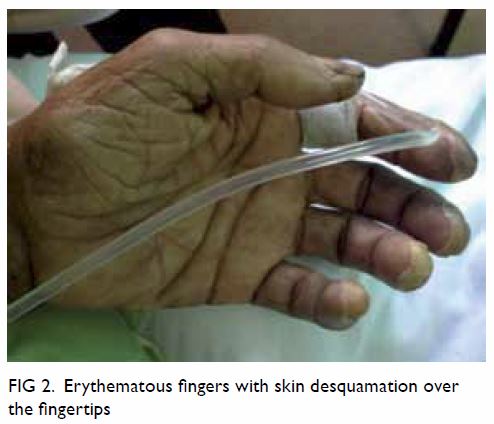
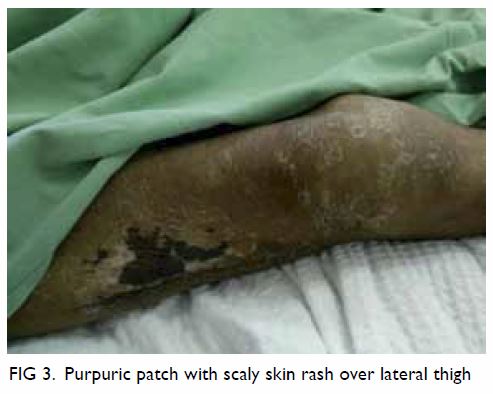
desquamation over the tips of the fingers (Fig 2), and a large purpuric patch over the lateral
aspect of both thighs (Fig 3) with generalised scaly dry skin over the
body.
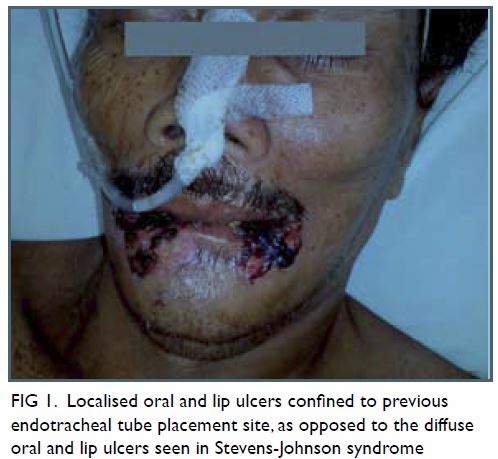
Figure 1. Localised oral and lip ulcers confined to previous endotracheal tube placement site, as opposed to the diffuse oral and lip ulcers seen in Stevens-Johnson syndrome
He was treated as Stevens-Johnson syndrome (SJS).
Antibiotic therapy was stopped and intravenous hydrocortisone was started
but his ulcers continued to worsen. A dermatological opinion was arranged
and revealed that the oral and tongue mucosa erosions were confined to the
site of previous endotracheal tube placement rather than being the diffuse
oral and lips erosions of SJS. Nikolsky sign was negative. The conjunctiva
was clear, and there was involvement of the nasal, urethral or anal
mucosa.
In view of the confined area of mucosa involvement,
he was diagnosed with medical device–related pressure ulcers. The purpura
and ecchymosis were due to the underlying coagulopathy secondary to septic
shock with DIC. Potential infective causes, eg vegetating herpes simplex,
staphylococcal scalded skin syndrome, were excluded by negative wound
culture. There were also no features of SJS on skin biopsy.
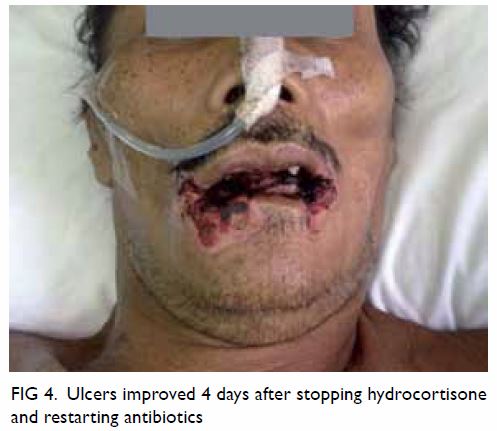
The steroid was stopped immediately and antibiotics
resumed. Albumin level was optimised. After 2 weeks of oral care, the
patient’s skin condition improved (Fig 4) and he finally attained full recovery.
Discussion
Tracheal intubation is one of the best methods of
airway protection1 but serious
complications may occur, especially in critically ill patients.2
Stevens-Johnson syndrome is part of a spectrum of
severe cutaneous adverse reactions that affect skin and mucous membranes.
It is commonly caused by certain medications or infections. Skin lesions
may be purpuric macule spots, erythema, or sometimes violaceous
target-like lesions. Mucous membrane erosions and ulcers almost always
appear in the eyes, mouth and lips, but may also occur in the upper
airway, genitourinary and gastrointestinal tract. Assessment is often
difficult when mucous membrane involvement is not yet apparent.3
Hypotensive episodes during septic shock may lead
to reduced perfusion pressure to the skin and mucosa. This may cause
pressure point areas to develop pressure sores.4
Hypoalbuminaemia and DIC may cause further deterioration of the ulcers.
Pressure sores are one of the most common complications among patients
undergoing mechanical ventilation in a poorly managed setting.5
Physicians should always be extra cautious when
diagnosing SJS. The consensus definition should always be consulted with
referral to a dermatologist or performance of a skin biopsy if there is
any doubt.3 An incorrect diagnosis
of SJS may lead to a totally inappropriate spectrum of treatment such as
cessation of appropriate life-saving antibiotics and the commencement of
steroid therapy that will increase the risk of infection and impair wound
healing.
References
1. International Liaison Committee on
Resuscitation. 2005 International Consensus on Cardiopulmonary
Resuscitation and Emergency Cardiovascular Care Science with Treatment
Recommendations. Part 4: Advanced life support. Resuscitation
2005;67:213-47.
2. von Goedecke A, Herff H, Paal P, Dörges
V, Wenzel V. Field airway management disasters. Anesth Analg
2007;104:481-3. Crossref
3. Mockenhaupt M. Severe drug-induced skin
reactions: clinical pattern, diagnostics and therapy. J Dtsch Dermatol Ges
2009;7:142-60. Crossref
4. Black JM, Edsberg LE, Baharestani MM, et
al. Pressure ulcers: avoidable or unavoidable? Results of the National
Pressure Ulcer Advisory Panel Consensus Conference. Ostomy Wound Manage
2011;57:24-37.
5. Tang WM, Tong CK, Yu WC, Tong KL,
Buckley TA. Outcome of adult critically ill patients mechanically
ventilated on general medical wards. Hong Kong Med J 2012;18:284-90.