Hong Kong Med J 2022 Jun;28(3):271.e1–2
© Hong Kong Academy of Medicine. CC BY-NC-ND 4.0
PICTORIAL MEDICINE
Liver and kidney toxicity caused by wild
mushroom poisoning
LF Yang, MD1; LP Zhu, MD1; YT Li, MD, PhD1; XB Zhong, MD1; ZG Chen, MD, PhD1; Karen KY Leung, MB, BS, MRCPCH2; KL Hon, MB, BS, MD2
1 Department of Pediatrics, The Third Affiliated Hospital of Sun Yat-sen University, Guangzhou, PR China
2 Department of Paediatrics and Adolescent Medicine, The Hong Kong Children’s Hospital, Hong Kong
Corresponding author: Dr KL Hon (ehon@hotmail.com)
In May 2020, a 2-year-old girl was admitted to our hospital with a 2-day history of persistent vomiting,
diarrhoea, abdominal pain, and headache. Her
family reported that she had eaten half of a large
mushroom, about the size of a palm (Fig a) 17 hours
before symptom onset.
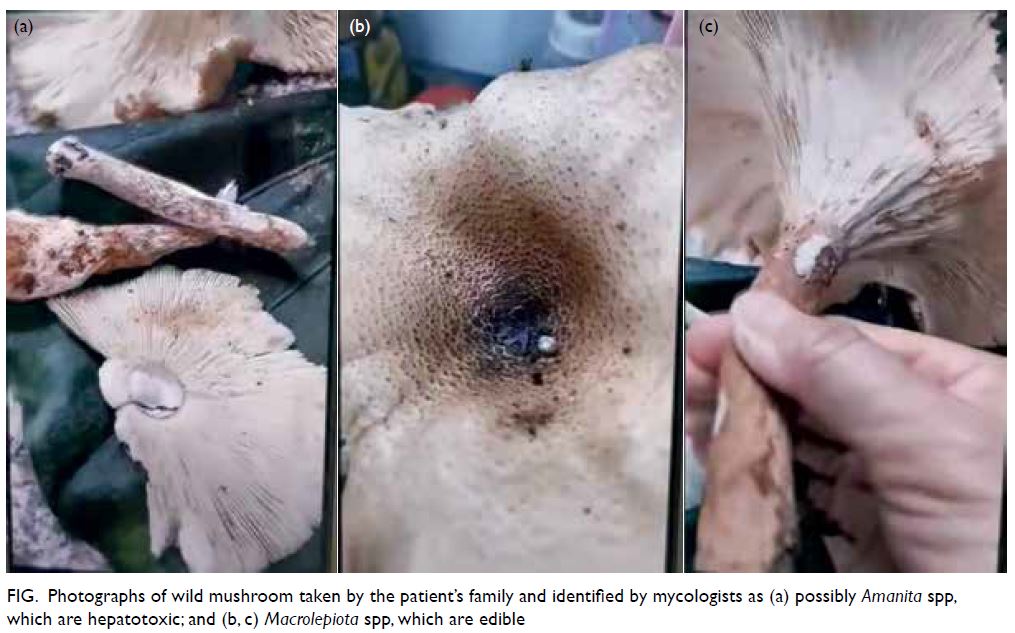
Figure. Photographs of wild mushroom taken by the patient’s family and identified by mycologists as (a) possibly Amanita spp, which are hepatotoxic; and (b, c) Macrolepiota spp, which are edible
Physical examination was unremarkable.
Laboratory investigations revealed liver disfunction,
with elevated aspartate transaminase (AST)
228 U/L and alanine transaminase (ALT) 211 U/L
rising to 2591 U/L and 2815 U/L, respectively. The
patient was admitted to the paediatric intensive care
unit for further treatment. After hospitalisation,
AST and ALT further increased to 4005 U/L and
4335 U/L, respectively. Plasma exchange was
performed along with treatments including 20%
albumin, high-dose penicillin, N-acetylcysteine
injection and Ganoderma lucidum. Liver function
gradually normalised over the following week and
the patient was discharged home.
The patient’s grandmother and aunt consumed
the other half of the same mushroom (Fig a) and other
mushrooms (Fig b and c), and both were admitted to hospital with serious vomiting, diarrhoea and
mild abdominal pain. Her aunt had normal liver
function and kidney function. The grandmother had
mild liver and renal impairment with AST 169 U/L,
ALT 147 U/L, blood urea nitrogen 12.1 mmol/L and
creatinine 168 μmol/L, made a rapid and recovery
following rehydration, a bicarbonate infusion,
furosemide, and hepatoprotective drugs for 3 days.
Cyclopeptides are the major lethal toxins
worldwide, often found in Amanita spp, Cyclospora
and galea.1 2 In Guangzhou from 2007 to 2011, the
most common species causing mushroom poisoning
was Amanita spp. In mainland China 95% of
fatal cases of mushroom poisoning are caused by
amanitin. In Hong Kong, 90% of wild mushrooms
are poisonous.
Ultra-performance liquid chromatography-mass
spectrometry has high accuracy, and good
sensitivity and specificity, and was used to identify
the toxin in our patient. However, it was already
2 days after the girl ate the wild mushrooms, and
the toxin might have been excreted so that the
concentration was too low for detection.
Prognosis is often poor for patients with long
incubation period of gastrointestinal symptoms
(>6 hr), early manifestations of liver and kidney
dysfunction, and multiple organ dysfunction.3 4
Plasma exchange effectively removes hepatotoxins
and improves survival, drugs such as silybin, N-acetylcysteine,
putatively ceftazidime/penicillin
and Ganoderma lucidum can also have a significant
benefit.5 Ganoderma lucidum contains triterpenoids
that can protect the liver and reduce oxidative stress
and apoptosis. Ganoderma lucidum decoction is
effective in the treatment of amanita poisoning at
a recommended dosage of 200 g/day decocted with
600 mL water, taking one-third of this decoction
(200 mL per dose) 3 times per day, for 7 to 14 days.
Liver transplantation is the final option for liver
failure caused by mushroom poisoning.
Mushroom poisoning is usually the result of
ingestion of wild mushrooms after misidentification
of a toxic mushroom as an edible species.
Public health education on identification of wild
mushrooms and the dangers of wild mushroom
consumption is particularly important to prevent
mushroom poisoning.
Author contributions
Concept or design: KL Hon, LF Yang.
Acquisition of data: LF Yang, LP Zhu.
Analysis or interpretation of data: YT Li, XB Zhong.
Drafting of the manuscript: LF Yang.
Critical revision of the manuscript for important intellectual content: ZG Chen, KKY Leung, KL Hon.
Acquisition of data: LF Yang, LP Zhu.
Analysis or interpretation of data: YT Li, XB Zhong.
Drafting of the manuscript: LF Yang.
Critical revision of the manuscript for important intellectual content: ZG Chen, KKY Leung, KL Hon.
All authors had full access to the data, contributed to the study, approved the final version for publication, and take responsibility for its accuracy and integrity.
Conflicts of interest
As an editor of the Journal, KL Hon was not involved in the peer review process. Other authors have disclosed no conflicts of interest.
Funding/support
This study received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Ethics approval
This study was approved by the Ethics Committee of The Third Affiliated Hospital of Sun Yat-sen University (Ref [2022]-02-064-01). Written informed consent was obtained from the
patient’s guardian for the publication of this case report and
all images.
References
1. Schenk-Jaeger KM, Rauber-Lüthy C, Bodmer M,
Kupferschmidt H, Kullak-Ublick GA, Ceschi A. Mushroom
poisoning: a study on circumstances of exposure and
patterns of toxicity. Eur J Intern Med 2012;23:e85-91. Crossref
2. Brandenburg WE, Ward KJ. Mushroom poisoning epidemiology in the United States. Mycologia
2018;110:637-41. Crossref
3. Trabulus S, Altiparmak MR. Clinical features and outcome of patients with amatoxin-containing mushroom poisoning. Clin Toxicol (Phila) 2011;49:303-10. Crossref
4. Bonacini M, Shetler K, Yu I, Osorio RC, Osorio RW.
Features of patients with severe hepatitis due to mushroom
poisoning and factors associated with outcome. Clin
Gastroenterol Hepatol 2017;15:776-9.Crossref
5. Lu Z, Hong G, Sun C, Chen X, Li H, Yu X. Chinese clinical guideline for the diagnosis and treatment of mushroom poisoning [in Chinese]. J Clin Emerg (China) 2019;20:583-98.

