© Hong Kong Academy of Medicine. CC BY-NC-ND 4.0
REMINISCENCE: ARTEFACTS FROM THE HONG KONG MUSEUM OF
MEDICAL SCIENCES
Journey through quantitative haematology
Dr Clarence CK Lam, FHKAM (Pathology), FHKCPath (Haematology)
Invited author, Hong Kong Museum of Medical Sciences
We tend to remember pathology, putting aside
autopsies and specimens which may not be
everybody’s cup of tea, as beautiful pictures captured
from histological sections under the microscope.
Pathology, in fact, has since many years ago evolved
beyond images. Something more precise with
minimal inter-observer difference is clearly more
desirable, and nothing is more precise than numbers.
Therefore, quantifying what we can see, grossly or
microscopically, remains one of the most important
missions of the pathologists.
Let us start with cell counting in haematology.
In modern clinical practice, full blood count is the
most basic haematology test provided by any decent
laboratory round the clock, and the results can be
generated by elaborate automated haematology
analyser systems literally within minutes according
to the clinical conditions of the patients. Hardly
can one imagine the enormous efforts and time
associated with a report on the ‘not-so-full’ blood
count before the advent of haematology analysers
based on the Coulter principle discovered by Wallace
H Coulter in the late 1940s for which a patent was
granted in 1953.
Blood counts were performed with a
haemocytometer in the good old days. The
haemocytometer, more commonly known in the
laboratory as a counting chamber, or simply the
chamber, was invented in the late 19th century. Its
invention is credited to Louis-Charles Malassez
(1842-1909), a French anatomist and histologist.
The most commonly used haemocytometer in the
haematology laboratory is the Neubauer counting
chamber, which is shown in Figure 1. This is a
generous gift from Professor James B Gibson to
the Hong Kong Museum of Medical Sciences, as
something that he himself had used in his earlier
career, and which he had carefully kept until his
retirement. It is essentially a thick glass microscopic
slide with a chamber of specific depth, etched
accurately at a defined dimension with a grid of
perpendicular lines. A properly positioned special
coverslip with certified thickness and flatness,
together with the best technique of loading an
appropriately diluted and thoroughly mixed blood
specimen by pipettes, ensures the precision of the
volume. By counting the number of cells in defined
areas of the haemocytometer, the number of cells
in a specific volume of the diluted blood specimen
is known. The concentration of cells in the blood overall, or cell counts, can be calculated by correcting for the dilution.
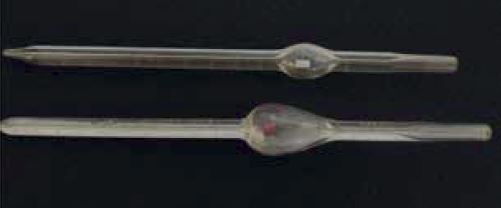
The graduated glass tubes with a bulge (Fig 2),
which harbours a little stirrer of either red or white,
are actually pipettes for diluting the peripheral blood
specimen and loading of the counting chamber: the
one with the red stirrer is for diluting the blood
specimen for counting of red cells while the white
is for leucocytes and platelets. These pipettes had
been routinely filled by suction by mouth through
a rubber tube until the risk of mouth pipetting
was recognised, and filling by aspirating with small
volume syringes was introduced. Different diluents
and dilutions, with which you are not going to be
bothered, are used for counting of different cell types.
After dilution and thorough mixing on a device and
discarding the portion of the specimen below the
bulge, the diluted blood specimen is loaded through
capillary action to the chamber. Any pressure will introduce too much specimen into the counting
chamber and result in an erroneous volume, thus a
wrong cell count. Counting under the microscope
will be performed after letting the loaded counting
chamber settle for a standard period of time, usually
5 to 10 minutes. If the loaded counting chamber is
left for too long before counting, the specimen may
evaporate and dry out, particularly in laboratories of
low humidity, thus affecting the distribution of the
cells, and resulting again in an erroneous result.
It is not difficult to imagine how tedious it was
to generate just one report on blood counts. It was
certainly a much more challenging task organising
a laboratory haematology service with such manual
tests. You would be surprised to learn that many a time
it was the house officers’ or the residents’ job to do the
blood counts. How different life was in the medical
profession just a few decades ago! Mind you, we have
yet to touch on the quality assurance measures which
are of pivotal importance in patient care. The prevailing
quality assurance framework then was understandably
inadequate when compared with the current concepts
and understanding of total laboratory management,
particularly concerning the requirements and
standards of laboratory accreditation. The first steps
to ensure ‘correctness’ of the results were to do the
tests in duplicate and standardise as far as possible the
various manual steps.
The last two decades of the 20th century
saw rapid evolution of cell counting technology.
Incorporating some relatively basic automation, this
evolution enabled comparatively high throughput
quality service, with remarkable accuracy and
precision, to cope with the increasing volume and
diversity of clinical service. Improvements in cell
counting technology, albeit in a more incremental
manner, are still seen in the first two decades of the
21st century. However, efficiency, with enhanced
workflow design and post-analytical software
support, and flexibility in setup, with large-scale or
modular automation to suit laboratory services of
variable complexities, have been the main foci of
development. These new automated analyser systems
also have built-in quality assurance capabilities to
cater for the requirements of accreditation.
The counting chamber is very seldom or
hardly ever used nowadays for blood counts in the
haematology laboratory because modern automated
haematology analyser systems have different modes
of analysis for accurately quantifying different cell
types in the peripheral blood should there be any
need. It is still being used in the clinical laboratory
setting for cell counting in different kinds of body
fluids. Even for this purpose, its use is again on a
downward trend, as new analysers can also cater for
cell counting of many body-fluid types.
I believe it is appropriate to share with you
some information about Professor Gibson, the donor of this artefact. Professor Gibson graduated
in 1943 from the University of Edinburgh and also
received his MD from Western Reserve University
at Cleveland, United States the same year. After
serving in the Royal Navy, during which he took part
in the Normandy landing, he worked on both sides
of the Atlantic before taking up an appointment as
Professor and Head of Department of Pathology
at The University of Hong Kong (HKU) from 1963
to 1983. He also served as Dean of the Faculty of
Medicine from 1972 to 1978. In addition to being a
world recognised expert in liver pathology, Professor
Gibson had contributed extensively in shaping and
driving for advancement in medical care in Hong
Kong through upgrading the standard of pathology
practice and service. It is largely due to the phenomenal
efforts and dedication of Professor Gibson that
pathology practice as we know today took its shape.
Professor Gibson established a separate Department
of Microbiology in 1968, set up an immunology
section and cytology service in the 1970s, set up a
tissue typing service, and oversaw the evolution of
the Clinical Biochemistry Unit into a separate unit
in the early 1980s. He also organised improvements
in various facilities. He is particularly remembered
for setting up a central electron microscope unit
in HKU and opening of a new Clinical Pathology
Building in Queen Mary Hospital in 1972. He was
instrumental in the formation of the HKU Hospital
Pathology Service in Queen Mary Hospital which
had provided a high-quality pathology service until
it was taken over by the Hospital Authority in the
1990s. Professor Gibson’s trainees were the first in
Hong Kong to pass the Royal College of Pathologists
Membership examination. Not only did pathologists
benefit from the foresight of Professor Gibson,
training of technical professionals throughout Hong
Kong was also upgraded through his oversight of the
establishment of a territory-wide medical laboratory
technician training programme, the Ordinary
and Higher Certificates in Medical Laboratory
Technology, via the Extramural Department (now
SPACE) of HKU. Professor Gibson received an
Honorary Doctorate of Science from HKU on his
retirement in 1983, and continued to keep an interest
in the pathology profession in Hong Kong after his
retirement and relocation to Scotland.
The haemocytometer has certainly done its due
in fulfilling its mission in the history of laboratory
haematology practice. It is an integral component of
the science and art of cell counting. It is a delight to
know that cell counting, although in areas outside
clinical laboratory practice, using a haemocytometer
can be automated!
Acknowledgement
I would like to thank Professor Faith CS Ho and
Professor SC Tso for their invaluable input.