© Hong Kong Academy of Medicine. CC BY-NC-ND 4.0
REMINISCENCE: ARTEFACTS FROM THE HONG KONG MUSEUM OF MEDICAL SCIENCES
The rigid bronchoscope: an obsolete instrument?
Moira Chan-Yeung
Member, Education and Research Committee, Hong Kong Museum of Medical Sciences Society
Until the era of bronchoscopy, inhalation of a foreign
body could result in a multitude of problems such
as chronic lung abscess, fistula formation, chronic
ill health and malnutrition, even death. Techniques
such as lobectomy or pneumonectomy had yet to
be developed to remove the affected lobe or lung.
Although instruments were available to inspect body
cavities such as the mouth, nose, ear, vagina, rectum
and urethra, inspection of the larynx and the trachea
presented great difficulties due to the lack of light.
Direct inspection of the airways became feasible
only after three major inventions: (1) instruments
for inspection, (2) suitable light sources, and (3)
adequate anaesthesia.
In 1854, the first problem was solved by Manuel
Garcia, a singing teacher in London, who observed
his own larynx using a dental mirror. Two years
later, a laryngologist Ludwig Turck used a dental
mirror for his work in the diagnosis and treatment
of laryngeal diseases. Nonetheless, the indirect
and reverse view of the anatomy posed difficulties
for most laryngologists. Surgery on the larynx was
also hindered by inadequate light and lack of local
anaesthesia.1
The first light source for inspection of body
cavities was invented in 1805 by a practitioner,
Philipp Bozzini, from Frankfurt. It consisted of a box
containing a candle, the light of which was reflected by
a hollow mirror into a split metallic tube. For organs
that could not be visualised by direct inspection,
he used this tube with a mirror to reflect the light
and image. The illumination from this awkward
light source, however, was poor and inadequate for
examination of the stomach and the airways. When
Thomas Edison invented the electric bulb in 1879,
and Mignon miniaturised it for distal illumination of
the endoscope, the reality of bronchoscopy became
a little closer. The second problem was solved.1
In 1884, Jellinek, a Viennese laryngologist, first
introduced cocaine that eliminated the reflexes of the
pharynx and the larynx and allowed passage of the
endoscope for inspection of the airways. The three
inventions were now in place and bronchoscopy
became a reality.1
In 1895, Gustav Killian in Mainz, Germany,
passed an endoscope through the larynx to the
bifurcation of the trachea in a tracheostomised
patient for the first time. He then practised on
corpses without tracheostomies to confirm his
previous observation that the bronchi were flexible
and elastic before he attempted the procedure on
healthy volunteers. In 1897, Killian removed the first
foreign body via the bronchoscope. He became well
known for his careful work after many publications
and lectures, and physicians from around the world
flocked to him to learn the techniques of rigid
bronchoscopy.1
Chevalier Jackson, from Philadelphia, was the
first to construct an ‘American bronchoscope’ with
a light carrier using a miniaturised electric mignon
bulb at the distal end and an extra suction channel.
In 1907, he published the first systematic textbook on
bronchoesophagoscopy and dedicated it to Killian,
the Father of Bronchoscopy. Jackson persistently
refused to patent his different inventions, instead
wanting them to be used as widely as possible—a
spirit to be emulated by the younger generation.2
In 1940, the optic telescope and in 1962, fibre
illumination were introduced to enhance the rigid
bronchoscope. From then on, rigid bronchoscopy
was used extensively for the diagnosis and treatment
of a number of lung diseases where lesions were in
the trachea or in the major airways.2
Broader application of bronchoscopy became
possible only after the development of flexible
instruments that could be easily introduced
under local anaesthesia. In 1964, when Shigeto
Ikeda from Japan first used a flexible fibre-optic
bronchoscope, he created quite a stir. The fibre-optic
bronchoscope received wide acclaim as a revolution
in bronchoscopy.
While the flexible fibre-optic bronchoscope
is now used routinely in most endoscopy units, and
a great many new inventions have been associated
with this instrument, the rigid bronchoscope still has
a place in the management of certain lung diseases.
For particular interventional procedures such as
laser and photodynamic laser therapy for lung cancer,
endobronchial stenting, and transtracheal puncture
of the carinal lymph nodes, the rigid bronchoscope
remains the preferred instrument for many clinicians
and investigators in Europe. The rigid bronchoscope
(Figure) is not obsolete but retains a vital place in
modern surgery.
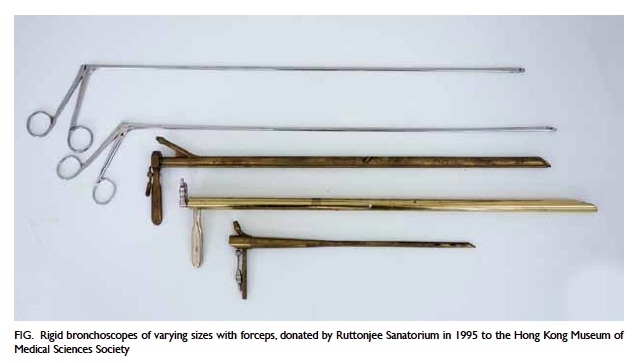
Figure. Rigid bronchoscopes of varying sizes with forceps, donated by Ruttonjee Sanatorium in 1995 to the Hong Kong Museum of Medical Sciences Society
References
1. Becker HD. Bronchoscopy: the past, the present, and the future. Clin Chest Med 2010;31:1-18. Crossref
2. Becker HD. A short history of bronchoscopy. In: Ernst A, editor. Introduction to bronchoscopy. New York: Cambridge University Press; 2009.

